Infection prevention and control protocols are essential for safety, but it’s important to recognise that gaps and risks can exist. Addressing these helps ensure strong compliance, reliable protection, and confidence in care.
Efficacy
Not all disinfectants are sporicidal, and in healthcare environments failing to use sporicidal disinfectants, particularly in high-risk areas, can have serious implications for patient safety and infection control.
Sporicidal disinfectants eliminate resilient pathogens such as Clostridioides difficile and Candidozyma auris (formerly Candida auris), which can survive on surfaces for extended periods and resist standard disinfectants. Without sporicidal action, these organisms can persist in the environment for months, increasing the risk of transmission via healthcare workers, equipment, or contaminated surfaces.
Combatting the risk:
Ensure your disinfectant has proven sporicidal efficacy by selecting products that meet rigorous standards such as EN 17126 and EN 17468. These efficacy test certifications confirm the product’s ability to eliminate bacterial spores which are among the most resistant pathogens in healthcare.
Dilution Rates Matter
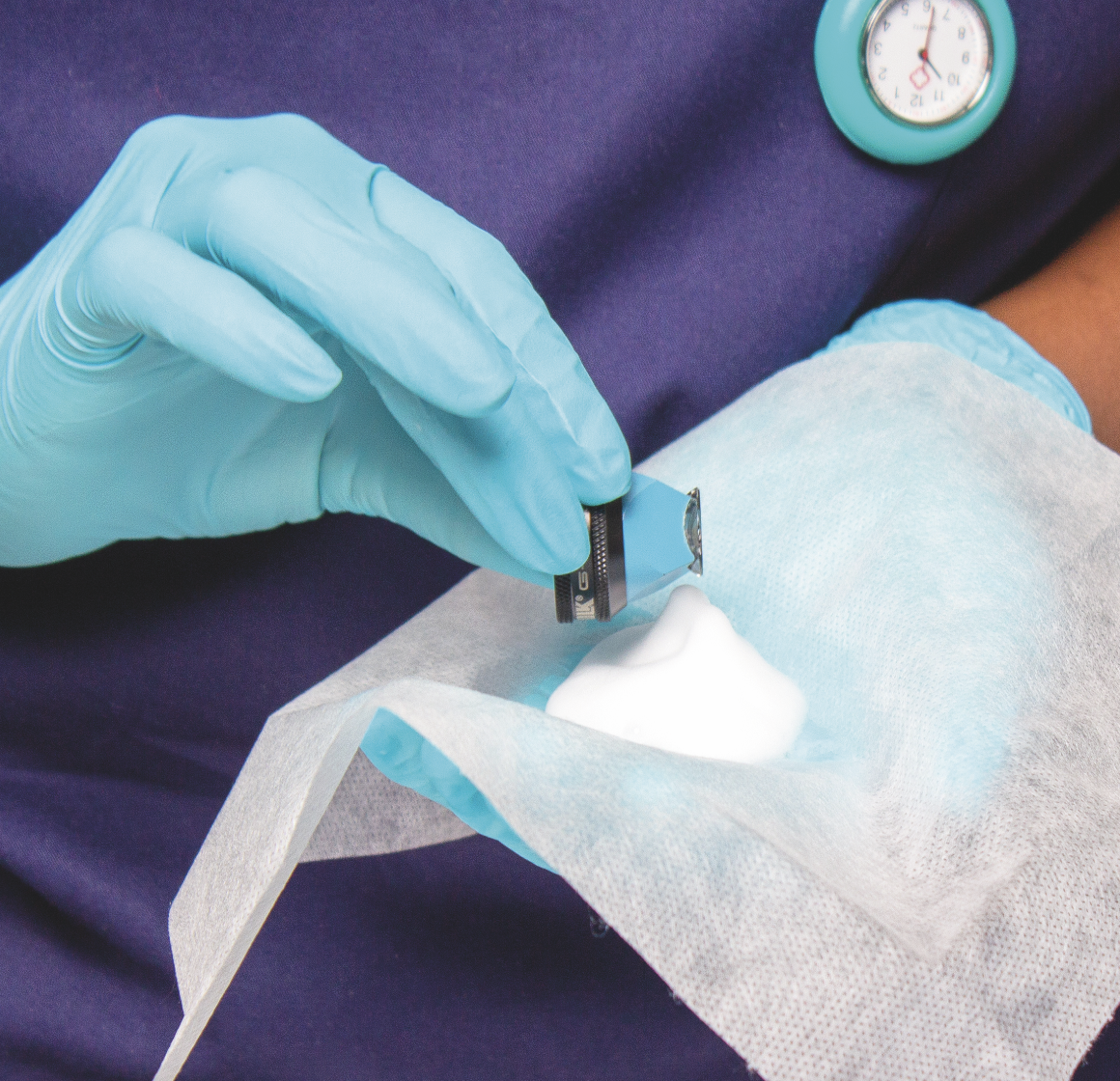
One often overlooked risk in infection prevention is the potential for human error when preparing disinfectant solutions, particularly with products which require precise dilution such as chlorine tablets. Chlorine tablets must be completely dissolved in specific volume of water to achieve the correct parts per million (ppm) concentration for disinfection.
Under-dilution (too little water) can lead to overly concentrated solutions, increasing the risk of surface damage, staff exposure, and unnecessary chemical use.
Over-dilution (too much water) is more concerning from an efficacy standpoint. It may result in sublethal concentrations that fail to kill spores, leaving surfaces inadequately disinfected. Worse, repeated exposure to sublethal doses can contribute to adaptive resistance mechanisms in microorganisms, potentially increasing the risk of antimicrobial resistance (AMR) over time.
Using pre-measured or ready-to-use sporicidal products can help mitigate these risks and ensure consistent, effective disinfection.

Combatting the risk:
Choose a disinfectant that comes in a ready-to-use format or features built-in dilution control. This eliminates the need for manual measuring, significantly reducing the risk of human error. By removing guesswork, you ensure consistent application and reliable efficacy.
Contact Times
Many high-level disinfectants have different contact times for different pathogens. For example, some disinfectants reach bactericidal efficacy in 1 minute, but require a 10-minute contact time to achieve sporicidal efficacy. Without clear protocols and training, this variability can lead to non-compliance and ineffective disinfection, increasing the risks of HAIs.

Combatting the risk:
Choose a disinfectant with a uniform and clearly defined contact time across all pathogen types. This simplifies training, reduces the chance of misuse, and ensures consistent efficacy, even in busy clinical environments. A single, reliable contact time helps staff apply protocols confidently and correctly, minimising the risk of premature drying or underexposure that could compromise infection control.
Reprocessing Times
Disinfectants with long contact times can slow down clinical workflows, especially in high-turnover areas. This can reduce throughput in a time of long waiting lists and healthcare settings under pressure. Long contact times can also lead to increased chemical exposure for staff, and potential surface damage and equipment wear.

Combatting the risk:
Select a disinfectant with a short, validated contact time that still delivers broad-spectrum efficacy. This helps to ensure high-level disinfection, even in fast-paced environments, reducing the risk of underexposure. Short contact times also streamline workflows and improve staff compliance.
Cost
Many automated systems for reprocessing medical devices require significant upfront investment, not only in the machines themselves but also in ongoing maintenance contracts, software updates, and staff training. These systems are designed to ensure consistent and validated cleaning and high-level disinfection, but the financial burden can be substantial.
There are also additional hidden operational costs, such as downtime due to machine servicing or repairs, the need for backup systems, plus energy and water consumption.

Combatting the risk:
Reduce financial and operational burden by choosing a manual disinfectant solution that requires no capital expenditure, service contracts, or utility consumption. Products that don’t rely on machines, water, or electricity offer a more predictable cost model and greater flexibility. This approach not only lowers upfront investment but also minimises ongoing maintenance and training costs.
Compatibility
Many high-level disinfectants, especially those with strong oxidising agents like chlorine or peracetic acid, can corrode metals, degrade plastics, and damage sensitive coatings. Over time, this can lead to:
- Cracking or warping of device components
- Clouding or etching of lenses and screens
- Reduced lifespan of reusable medical equipment
This not only increases replacement costs but can also affect device performance, potentially leading to inaccurate readings or mechanical failure.
Combatting the risk:
Choose a disinfectant that is material-compatible and validated for use on the surfaces and devices in your facility. This helps prevent corrosion, discoloration, and mechanical damage. Using a product with proven compatibility protects your assets, maintains device performance, and reduces costly repairs or replacements due to chemical wear.
Hidden risks in infection prevention can quietly compromise even the most robust protocols. By choosing the right products and practices, you can safeguard both patient safety and operational efficiency.